Jakarta’s Air Pollution, and the New Emerging Cause for Skin Aging
Ruri D. Pamela
Department of Dermatology, Dr. Suyoto Hospital Ministry of Defense, Jakarta, Indonesia
Abstract
Air pollution as an impact of modern urbanization and industrialization continues to increase and has become a global problem. The human skin organ acts as a barrier and frontline to external environment, so it is frequently directly exposed to pollution. A Greenpeace report released in early 2019 listed Jakarta as South Asia’s most polluted city. The effect of major air pollutants such as nitric oxide, polycyclic aromatic hydrocarbons, volatile organic compounds, and particulate matter to human skin has been investigated in few studies. This article reviews how air pollutants currently perceived as a major cause of skin aging through their mechanism in damaging skin barrier and increase accumulation of reactive oxygen species.
Introduction
Skin damage caused by ultraviolet radiation from the sun has long been recognized as one of the main cause for aging for the last 20-30 years. Now we believe environmental exposure of air pollution is a new emerging problem that we will face for the next few decades. Air pollution is the greatest environmental risk to health today. New data from World Health Organization (WHO) in 2018 shows that 9 out of 10 people breathe air containing high levels of pollutants. Updated estimations reveal an alarming death toll of 7 million people every year caused by ambient (outdoor) and household air pollution1. Numerous clinical and epidemiological studies have highlighted the adverse effects of environmental pollutants on health2. Jakarta is one of the capital cities in south east Asia and this has become a growing concern in today’s society since the city has been making frequent appearances on the list of global cities with the worst air conditions3. The highest exposure to ambient air pollutants in Indonesia (including Jakarta as the most urban area) is attributable to motor vehicles. The index of air pollution in 2007 using Air Quality Monitoring System shows the status “good day” in Jakarta for only 72 days and 29 days in 2017.
Environmental contaminants also have a negative impact on the skin, which is the largest organ in the human body and one of the most important barriers against pollution4,5. Even though not many publications and scientific studies describe the impact of air pollution on skin integrity, this potential hazard should get our attention. Since the skin acts as a barrier between the organism and the environment, it is frequently directly exposed to pollution.
Aging is the result of a complex interaction of biological, physical, and biochemical processes that cause changes and damage to molecules, cellular function, and organs6. Skin aging is caused by two main processes: extrinsic aging due to environmental factors and intrinsic aging due to time. Many publications suggest that intrinsic aging is related to the accumulation of cellular damage from the active oxygen radicals in the body7,8. A relationship between air pollution and skin aging was first shown in the SALIA study, an epidemiological study of elderly Caucasian women, which indicated that exposure to traffic related particulate matter (PM) contributes to skin aging9-11. Another study also showed that prolonged or repetitive exposure to high levels of air pollutants may have profound negative effects on the skin12.
Common Air Pollutants
WHO defines pollution as contamination of the indoor or outdoor environment by any chemical, physical or biological agent that modifies the natural characteristic of the atmosphere1. Pollutants can be inhaled, ingested, or come into contact with the skin depending on the form in which they occur13. The majority of outdoor pollutants come from anthropogenic sources such as vehicle emissions, fossil fuel combustion, forest fires, and industrial processes2,9. The main sources of pollutions are particulate matter (PM), polycyclic aromatic hydrocarbons (PAHs), volatile organic compounds (VOCs), nitrogen, sulfur dioxides, carbon monoxide, ozone, and heavy metals4,7,12,13. Other environmental air pollutants of major public concern include activation of aryl hydrocarbon receptors (AhR)2. AhR is a ligand-activated transcription factor found in various skin cells including keratinocytes, fibroblast and melanocytes. Non-activated AhR resides in a cystosolic multiprotein complex and upon ligand binding, the complex dissociates, causing AhR translocation to the nucleus where it stimulates gene expression. Activation of AhR plays a role in mediating biochemical and toxic effects of air pollutants and causing cell biological growth and differentiation2,12.
Particulate matter represents another environmental threat to which millions of humans worldwide are exposed10. It is a complex mixture of liquid and/ or solid droplets suspended in gas14. Coarse particles (PM10) are between 2.5-10 mm in diameter. They are components of dust, soil, and dusty emission from various industries. Fine particles (PM2,5) measure < 2.5 mm in diameter and are emitted from open fires, power plants and automobile exhaust15. PAHs are generated by traffic- or industry-related incomplete combustion processes and found in soot exposure11. Furthermore, PAHs have shown the strongest association for the formation of acquired pigment spot in human skin based on epidemiological studies16. Long term-exposed skin to PM-bound PHAs either through hair follicle or transepidermal absorption may lead to oxidative stress and skin aging12,19. VOCs originates from the use of organic solvent in paints, varnishes (e.g. aliphatic hydrocarbons, ethyl acetate, glycol ethers, methylene chloride, and acetone), vehicle refinishing products, tobacco smoke, stored fuels, exhaust from cars and emissions from industry12. Ground level ozone (O3) generation is a major component of smog and is formed as a result of a photochemical reaction between oxygen and pollutants such as VOCs which is facilitated by sunlight, also called summer photochemical smog2,12.
The effects of nitrogen dioxide (NO2) on human skin have been investigated by Huls et al in a large cohort study in the Asian and Caucasian populations. Exposure to NO2 was significantly associated with more lentigines on the cheeks in both cohorts10,11. In the Asian population, lentigines formation is considered to be a hallmark of skin aging. Activation of AhR signaling in human skin through exposure to air pollutant, especially PAHs will cause a crosstalk of dermal fibroblast and epidermal keratinocytes with melanocytes. On the other hand, prolonged exposure to PAHs-loaded air pollutants directly damages macromolecular structures in fibroblast and keratinocytes, and activation of melanocytes16.
WHO recommends an annual mean exposure threshold of 10 µg/m3 to minimize the risk of health impacts from PM2.5. PM2.5 is a representative measures of air pollution and it refers to particulate matter (ambient airborne particles) which measure up to 2.5 microns in size and are able to penetrate deep into human respiratory system causing a wide range of short and long-term health effects. The mean exposition of Jakarta’s air pollution to PM2.5 is 45.3 µg/m3 and it is considered as “unhealthy for sensitive groups”1. This measurement using real time Air Quality Index (AQI) is provided by the Indonesian Department of Meteorology, Climatology, and Geophysics using standardized air quality monitoring devices placed at several points. An AQI is measured based on five pollutants: particulate matter, sulfur dioxide, carbon monoxide, nitrogen dioxide, and ozone.
Lefebvre et al. published a study about the impact of urban pollution on skin quality, and they found that there is a tendency to find more skin problems such as urticarial and atopy disease in the more polluted zone (Mexico City) compare to the less polluted zone (Cuernavaca)17.
Possible Mechanism of Action
Particulate matter (PM) smaller than 0,1 µm were able to enter the skin tissue18 and penetrate either through hair follicles or transepidermally19. A major mechanism by which PM exerts its detrimental effects is through the generation of oxidative stress, an important contributor to extrinsic skin aging, as shown in Figure 120. These nanoparticles from PM not only cause oxidative stress in part of their physical properties, but also can serve as carriers for organic chemicals and metals that are capable of localizing in mitochondria and generating reactive oxygen species (ROS)10. Accumulation of oxidative stress by the excessive ROS in the body causes DNA damages and cellular signaling disruptions, resulting in the dysregulation of immune systems and induction cascade of inflammation7,21.
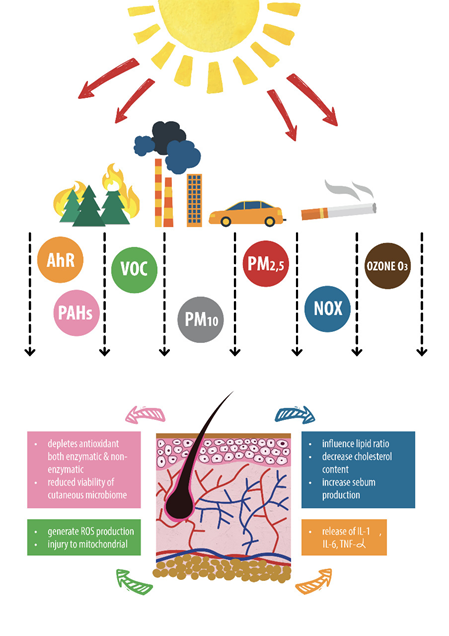
Ahr: aryl hydrocarbon receptors; PAHs: polycyclic aromatic hydrocarbons; VOC: volatile organic compounds;
PM: particulate matter; NOx: nitric oxide; ROS: reactive oxygen species; IL: interleukin; TNF: tumor necrosis factor
Figure 1: Skin damage mechanism related to pollutants
Pollutants induce stratum corneum (SC) modification and seems to cause additive oxidative stress in stratum corneum17,22. Most penetration occurs through lipid-rich intercellular regions, and very lipophilic molecules often have the highest penetration5. The environmental contaminant influence composition of skin lipids as the ratio of lipids is disturbed, the cholesterol content is decreased, while the sebum secretion rate is higher4.
Ozone pollutant is a highly reactive compound that generates free radicals and depletes antioxidants in the epidermis14,23. Two studies conducted in murine stratum corneum demonstrates that ozone depletes both enzymatic and non-enzymatic antioxidant reserves in the skin, such as uric acid, vitamin C, tocopherol, glutathione14,24,25. Indeed, a study by McCarthy et al. shows normal human epidermal keratinocytes (NHEK) exhibit high release of interleukin (IL)-1α above basal level as a response to ozone exposure. This elicitation of a pro-inflammatory response by the increase in IL-1α may trigger the immune function of the skin and may induce further damage26. On the other hand, metal constituents from the pollutant particles can serve as organic compounds carriers like PAHs which are highly lipophilic27 and contribute to mitochondrial injury and generate ROS production28. It also has been observed that prolonged exposures to particulate matter increase release of systemic proinflammatory cytokines such as IL-6 and TNF-α27,29.
The impact of key pollutants also has been shown to alter skin microbiome. Resident cutaneous microbiome is increasingly viewed as an integral part of the functional unit of the skin and plays an important role in homeostatic regulation30. Previous studies showed that in-vivo human skin exposure to ozone was significantly reduced the viability of natural flora14,31.
Implications for Dermatological Practice
People all over the world are exposed to many key pollutants and particulate matter that readily challenge the quality of their skin on a daily basis. Urban life also makes it impossible to avoid both indoor and outdoor pollutants that are harmful, have the potential to accelerate the normal aging process, and act as a trigger to skin allergies. The growing awareness and concern about the impact of air pollution to the skin has increased the demand of “anti-pollution cosmetics” and there is as well need a need for proper assays to evaluate the anti-pollution efficacy4. There are no established guidelines currently available for protecting the skin against air pollution14.
Recently, skin protection against air pollution should focus on repairing the epidermal barrier, optimization of antioxidant reserve, and reducing inflammation caused by air pollutants14. Repairing the epidermal barrier includes a strategy to reduce particle load on skin, such as suggestion to use rinse-off products9,32. Daily photoprotection with sunscreen is another important thing as UV radiation may potentiate the deleterious effects of pollutant particles on the skin9. Improvements in skin barrier function also include regular use of emollients to reduce transepidermal water loss32.
As mentioned before, particulate matter as major air pollutants will cause excessive reactive oxygen species and generate oxidative stress33. Application of topical antioxidants in daily manner can be a strategy to reduce the harmful effects of air pollutants on skin32.
Conclusion
Currently, our knowledge regarding the effects of air pollution on skin remains limited, more research is needed for better understanding of the link between air pollution and its mechanism to skin aging. Further studies are required to assess the effects of air pollution on the skin of short and long term exposure. Application of topical antioxidants to protect skin from pollutants also needs more research to optimize its use and to answer how much is needed to inhibit the harmful effects.
References
- The IQAir, Air Visual. 2018 World Air Quality Report. 2018.
- Koohgoli, Roxanna. "Bad air gets under your skin." Experimental dermatology. 2017; 26(5): 384-387.
- KS. 2019 August 1. Jakarta records worst air quality in the world again. Channel News Asia. Available at: https://www.channelnewsasia.com/news/asia/jakarta-air-quality-worst-in-the-world-again-indonesia-11772442
- Rembiesa J, Ruzgas T, Engblom J, et al. The impact of pollution on skin and proper efficacy testing for anti-pollution claims. Cosmetics. 2018; 5: 4.
- Goldsmith, Lowell A. "Skin effects of air pollution." Otolaryngology--Head and Neck Surgery. 1996; 114(2): 217-219.
- Schulze C, Wetzel F, Kueper T, et al. Stiffening of human skin fibroblast with age. Clin Plast Surg. 2012; 39(1): 9-20.
- Kim KE, Cho D, Park HJ. Air pollution and skin diseases: Adverse effects of airborne particulate matter on various skin diseases. Life Sciences. 2016; 152: 126-34.
- Farage, MA, Farage KW, Miller P, et al. Characteristics of the Aging Skin, Adv. Wound Care New Rochelle. 2013; 2: 5–10.
- Krutmann, Jean. "The skin aging exposome." Journal of dermatological science. 2017; 85(3): 152-161.
- Vierkotter A, Schikowski T, Ranft U, et al. Airborne particle exposure and extrinsic skin aging. J Invest Dermatol. 2010; 130(12): 2719-26.
- Huls, Anke. "Traffic-related air pollution contributes to development of facial lentigines: further epidemiological evidence from Caucasians and Asians." The Journal of investigative dermatology. 2016; 136(5): 1053.
- Drakaki E, Dessinioti C, Antoniou CV. Air pollution and the skin. Front Environ Sci. 2014; 2: 1-6.
- Baudouin C, Charveron M, Tarroux R, et al. Environmental pollutans and skin cancer. Cell Biol Toxcol. 2002; 18: 341-8.
- Mancebo SE, Wang SQ. Recognizing the impact of ambient air pollution on skin health. JEADV. 2015; 29: 2326-32.
- Kampa M, Castanas E. Human health effecs of air pollution. Environ Pollut. 2008; 151: 362-7.
- Nakamura M, Morita A, Seité S, et al. Environment-Induced Lentigines (EILs): Formation of solar lentigines beyond ultraviolet radiation. Exp Dermatol. 2015.
- Lefebvre MA, Pham DM, Boussouira B, et al. "Evaluation of the impact of urban pollution on the quality of skin: a multicentre study in Mexico." International journal of cosmetic science. 2015; 37(3): 329-338.
- Tinkle SS, Antonini JM, Rich BA, et al. Skin as a route of exposure and sensitization in chronic beryllium disease. Environ Health Perspect. 2003; 111: 1202–1208.
- Lademann J, Otberg N, Jacobi U, et al. Follicular penetration and targeting. J Investig Dermatol Symp Proc. 2005; 10: 301–3.
- Schroeder P, Lademann J, Darvin ME, et al. Infrared radiation-induced matrix metalloproteinase in human skin: implications for protection. J Invest Dermatol. 2008; 128(10): 2491-2497.
- Godic A, Poljšak B, Adamic M, et al. The role of antioxidants in skin cancer prevention and treatment. Oxidative Med Cell Longev. 2014; 2014: 860479.
- Valacchi G, Weber SU, Luu C, et al. Ozone potentiates vitamin E depletion by ultraviolet radiation in the murine stratum corneum. FEBS Lett. 2000 Jan 21; 466(1): 165-8.
- Cotovio J, Onno L, Justine P, et al. Generation of oxida- tive stress in human cutaneous models following in vitro ozone exposure. Toxicol In Vitro. 2001; 15: 357–362.
- Weber SU, Thiele JJ, Cross CE, et al. Vitamin C, uric acid, and glu- tathione gradients in murine stratum corneum and their susceptibility to ozone exposure. J Invest Dermatol. 1999; 113: 1128–1132.
- Thiele JJ, Traber MG, Polefka TG, et al. Ozone-exposure depletes vitamin E and induces lipid peroxidation in murine stratum corneum. J Invest Dermatol. 1997; 108: 753–757.
- McCarthy JT, Pelle E, Dong K, et al. Effects of ozone in normal human epidermal keratinocytes. Exp Dermatol. 2013; 22: 360–361.
- Magnani ND, Muresan XM, Belmonte G, et al. Skin damage mecha- nisms related to airborne particulate matter exposure. Toxicol Sci. 2016; 149(1): 227–236.
- Li N, Xia T, Nel AE. The role of oxidative stress in ambient particulate matter induced lung diseases and its im- plications in the toxicity of engineered nanoparticles. Free Radic Biol Med. 2008; 44: 1689–1699.
- Marchini T, Magnani ND, Paz ML, et al. Time course of systemic oxidative stress and inflammatory response induced by an acute exposure to Residual Oil Fly Ash. Toxicol Appl Pharmacol. 2014; 274: 274–282.
- Prescott SL, Larcome DL, Logan AC, et al. The skin microbiome: impact of modern environtments on the skin ecology, barrier integrity, and systemic immune programming. World Allergy Organization Journal. 2017; 10: 29.
- He QC, Tavakkol A, Wietecha K, et al. Effects of environmentally realistic levels of ozone on stratum corneum function. International Journal of Cosmetic Science. 2006; 28(5): 349–357.
- Krutmann J, Liu W, Li L, et al. "Pollution and skin: from epidemiological and mechanistic studies to clinical implications." Journal of dermatological science. 2014; 76(3) 163-168.
- Valacchi G, van der Vliet A, Schock BC, et al. Ozone exposure activates oxidative stress responses in murine skin. Toxicology. 2002 Sep 30; 179(1-2): 163-70.
